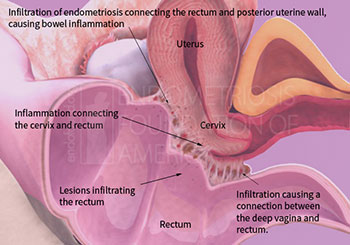
Bowel Endometriosis
Bowel endometriosis is a more advanced form of the disease in which endometrial-like tissue grows on or within the intestines, most commonly the rectum and sigmoid colon.
This can cause significant digestive and pelvic symptoms that often resemble irritable bowel syndrome (IBS) or gastrointestinal infections.
Because of this, many women remain undiagnosed for years, making expert evaluation extremely important.
The severity of symptoms depends on the depth of invasion and the extent of adhesions.
Women may experience pelvic pain, bowel discomfort, or cycle-related digestive issues.
In moderate-to-severe cases, the bowel may become narrowed, causing difficulty in passing stools or chronic constipation.
Common Symptoms of Bowel Endometriosis
Symptoms frequently worsen around menstruation but may also persist throughout the month.
Recognizing these signs can help in early diagnosis and intervention.
- Painful bowel movements: Especially during periods.
- Constipation or difficulty passing stools: Sometimes with a feeling of incomplete evacuation.
- Diarrhea or alternating constipation and loose stools: Often mistaken for IBS.
- Pelvic or lower abdominal pain: May be chronic or cycle-related.
- Bloating and abdominal heaviness: Worsening near menstruation.
- Pain during intercourse: Particularly with deep penetration.
- Rectal bleeding: Rare, but can occur during menstruation.
- Nausea, fatigue, and digestive upset: Especially during periods.
How Bowel Endometriosis Is Diagnosed
Proper diagnosis requires a combination of gynecologic assessment and advanced imaging.
Since bowel involvement can be subtle and difficult to detect, evaluation by a specialist in deep infiltrating endometriosis is important.
- Pelvic examination: May reveal tenderness or restricted organ mobility due to adhesions.
- Transvaginal ultrasound: Useful in detecting nodules, endometriomas, or bowel thickening.
- MRI pelvis: Highly effective for mapping deep infiltrating endometriosis and bowel involvement.
- Diagnostic laparoscopy: The most accurate method for confirming the condition and treating nodules simultaneously.
- Colorectal evaluation (if needed): Sometimes recommended for severe cases to check the extent of bowel narrowing.
Treatment Options
Treatment is tailored based on symptom severity, depth of bowel involvement, and fertility goals.
Advanced laparoscopic or robotic surgery is often preferred for precise removal and to minimize complications.
- Medical management: Hormonal therapy may help control symptoms in early or mild cases.
- Laparoscopic excision surgery: Removes endometriotic nodules while preserving bowel function.
- Shaving technique: Superficial disease is removed without entering the bowel.
- Discoid excision: A small disc-shaped portion of bowel wall is removed for deeper lesions.
- Segmental resection: Required in severe cases where a larger segment of bowel is affected.
- Fertility-sparing approach: Treatment is planned carefully for women wishing to conceive.
Minimally invasive surgery performed by an experienced surgeon offers the best outcomes—faster recovery, fewer complications,
and long-lasting symptom relief. A multidisciplinary team may be involved for complex cases to ensure safe and complete treatment.
Benefits of Early & Expert Treatment
- Improved bowel function and relief from painful symptoms
- Lower risk of disease progression or bowel obstruction
- Better fertility outcomes and preserved pelvic anatomy
- Reduced recurrence when surgery is done accurately
- Enhanced quality of life and daily comfort
If you experience persistent digestive discomfort, pelvic pain, or symptoms that worsen around your periods,
evaluation for bowel endometriosis is essential. With advanced diagnostic tools and minimally invasive expertise,
effective treatment and long-term relief are absolutely achievable.